Allergies: Disease Overview
Allergies are one of the most common immune system conditions, impacting as many as one in five people. Common allergies include pollen, animal dander, dust, and foods including nuts, shellfish and milk.
At BRI, our allergy research includes understanding the cells that cause allergies and exploring therapies that can stop allergies or reduce sensitivity to allergens. We also study immune system diseases linked to allergies including eosinophilic esophagitis (EOE) and celiac disease.
What Are Allergies?
Allergies happen when your immune system reacts too strongly to a foreign substance, like mold, pet dander, insect bites or stings, or certain foods. People who don’t have allergies can come into contact with these substances and have no reaction, while people with allergies may sneeze, develop a runny nose, or experience swelling and rashes. In severe cases, people can experience anaphylaxis, a life-threatening medical emergency where the blood pressure drops suddenly and the airways narrow, making it difficult to breathe.
What Causes Allergies?
Allergies are rooted in an overactive immune system. While the immune system is supposed to fight off harmful invaders like viruses and bacteria, sometimes it gets confused and starts attacking when it shouldn’t. For example, in people who are allergic to pollen, their bodies sense pollen and get ready to fight — causing a runny nose, sneezing and other defenses meant for germs like viruses.
Scientists, including those at BRI, are still working to understand exactly what causes allergies and why some people develop allergies and others don’t. Genetics likely play a role in allergies, and people with a close family member with allergies are more likely to develop them. Environmental factors like air pollution or mold can also influence the likelihood of developing allergies.
What Is the Latest Research Into Allergies?
BRI's current research includes:
- Understanding why some people develop allergies and others don’t.
- Lab research into cells or processes to target to treat allergies.
- Clinical trials that use immunotherapies that aim to make children with peanut allergies less sensitive to peanuts.
- Exploring Th2A cells, a cell type discovered at BRI that plays a role in all allergies. Researchers are seeking ways to target these cells to reduce allergy symptoms or stop allergies altogether.
- Understanding the role allergies play in eosinophilic esophagitis (EOE), a rare immune system condition that’s connected to food allergies and causes serious inflammation in the esophagus.
Labs studying allergies
Altman Lab
The Altman lab focuses on use of whole genome transcriptional profiling and multi-omics approaches, and leverages big-data computational biology to understand the molecular mechanisms underpinning severe asthma and other immunologic diseases.
Campbell Lab
The Campbell laboratory is interested in understanding the basis for T cell activation, function and tolerance.
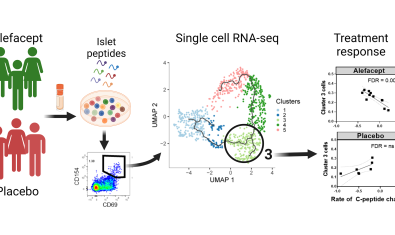
Cerosaletti Lab
Dr. Cerosaletti’s research is focused on the role of the adaptive immune system in the development and progression of immune mediated diseases and the response to treatment.
Kwok Lab
The Kwok lab uses tetramers and other antigen specific T cell assays to examine autoreactive T cells in autoimmune diseases in order to provide insights into disease mechanisms and identify strategies for disease intervention.
Clinical Research Studies in Allergies
Studies labeled as “Enrolling” are actively recruiting new participants while studies labeled as “Closed to Enrollment” are still active but no longer seeking new participants.
Please email the Clinical Trials Unit or call (206) 287-6260 for more information.
- A Phase 2, Open Label Extension Study to Evaluate Long Term Safety and Clinical Activity of Briquilimab in Participants From Jasper Sponsored Chronic Urticaria Trials.
Learn more at Clinicaltrials.gov
Principal Investigator: Rahool Davé, MD
Status: Enrolling- A Phase 3, Double-blind, Placebo-controlled, Randomized Study to Assess the Efficacy and Safety of Epicutaneous Immunotherapy with DBV712 250 μg in 4-7-year-old Children with Peanut Allergy (VITESSE)
Learn more at Clinicaltrials.gov
Principal Investigator: Rahool Davé, MD
Status: Closed to Enrollment- A Phase 1b/2a, Dose Escalation Trial of Safety, Pharmacokinetic/Pharmacodynamic and Preliminary Clinical Activity of Briquilimab in Adult Patients with Chronic Spontaneous Urticaria (CSU) Who Remain Symptomatic Despite Treatment with Omalizumab
Learn more at Clinicaltrials.gov
Principal Investigator: Rahool Davé, MD
Status: Closed to Enrollment