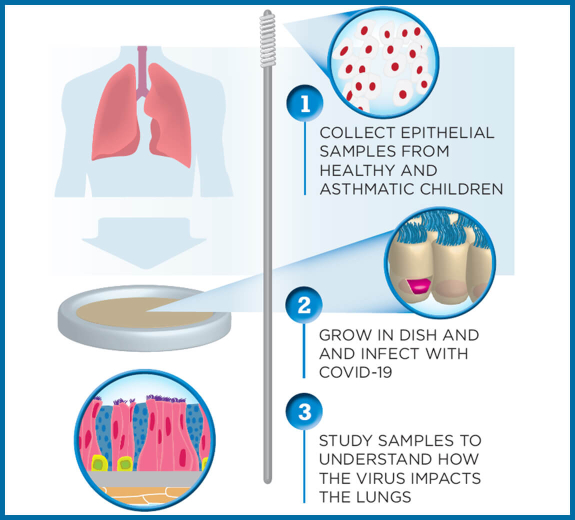
How does your body respond to different strains of coronavirus?
Bill Kwok, PhD, is on a quest to learn more about how the T cells in your immune system respond to different strains of the virus. His team hopes to learn if various strains of the virus lead to different immune responses and whether these different immune responses are correlated with clinical symptoms.
“Understanding what’s different about the immune system reaction, especially in people with more severe symptoms, could help us design treatments to fight off the virus,” Dr. Kwok says.
Why does the immune system go into overdrive?
Some COVID-19 patients have mild symptoms at first, then get significantly sicker a few days later. Their oxygen levels plummet and they may even need a ventilator.
Many researchers including BRI’s Jessica Hamerman, PhD, believe this response could happen because of an immune system response called a cytokine storm. Cytokines are proteins that are supposed to help your immune system fight off invaders like bacteria and viruses — they act like a fire alarm calling in immune cells to fight the infection. When the infection is gone, the fire alarm goes off and your immune system relaxes. But Dr. Hamerman likens a cytokine storm to a fire alarm that won’t turn off — your immune system keeps calling in more firefighters, even when the fire is out.
“The firefighters keep coming, spraying water and doing a lot of damage to your home if the alarm never stops,” she says. “Similarly, the cytokines keep calling in immune cells that make a lot of toxic molecules that can cause tissue damage and severe problems like pneumonia. The virus isn’t making these patients sick — it’s their immune system’s response to the virus.”
Dr. Hamerman recently earned a grant to study this response, working with several collaborators including Virginia Mason’s Uma Malhotra, MD, BRI’s Carmen Mikacenic, MD, and BRI Biostatistician Tee Bahnson.
“We already have some tools for treating cytokine storms when they’re triggered by autoimmunity, by other infections or when caused by a genetic condition—a set of syndromes called hemophagocytic lymphohistiocytosis (HLH),” Dr. Hamerman says. “We want to see how similar these responses are and if biomarkers that inform therapies for HLH patients will also work for cytokine storms caused by COVID-19.”
Can we find better treatments for severe COVID-19?
Long before the pandemic, Carmen Mikacenic, MD, had to tell many patients and families that going on a ventilator was their only hope — and there was no way to predict if it would work. Now, many patients with severe COVID-19 are hearing the same thing and Dr. Mikacenic wants to be able to give them better answers.
Dr. Mikacenic, BRI’s newest principal investigator who comes to us from the University of Washington, is a pulmonologist and critical care doctor. She treats patients with lung problems like acute respiratory distress syndrome (ARDS). ARDS is a condition where fluid collects in the lungs, making it hard or impossible to breathe. It’s also a common COVID-19 complication.
“We put patients on ventilators to support them while their body fights off the disease, but we don’t have therapies to fix the underlying condition,” Dr. Mikacenic says.
That’s why she’s on a quest to learn more about why people develop ARDS, how to better predict their outcome, and find new treatment options. She’ll be receiving a grant to learn more about how ARDS affects patients including those with COVID-19.
“When someone develops ARDS, I want to be able to tell their family if a ventilator will help and, eventually, that we have a treatment to address what’s causing their lung problem,” Dr. Mikacenic says. “This research brings us closer to that.”